Габапентин, спочатку розроблений для лікування судом, стає все більш поширеним засобом полегшення різних видів болю. Кількість рецептів зросла на 150% з 2010 року, досягнувши 73,1 мільйона у 2024 році. Це зростання не випадкове: агресивний маркетинг, більш широке позареєстрове застосування (призначення для станів, не схвалених FDA) і прагнення знизити залежність від опіоїдів відіграють свою роль. Але чи справді габапентин ефективний при полегшенні болю і кому слід його розглянути?
Що Таке Габапентін і Чому Він Так Популярний?
Габапентин (продається під торговими марками, такими як Neurontin, Gralise та Horizant) схвалений FDA для трьох станів: часткові судоми, постгерпетична невралгія (нервовий біль після лишаю, що оперізує) і синдром неспокійних ніг. Однак він часто призначається “поза інструкцією” для інших видів болю, включаючи фіброміалгію, синдром подразненого кишечника і навіть біль у спині.
Перехід до габапентину частково зумовлений скороченням призначень опіоїдів за хронічного болю. Лікарі шукають альтернативи, і габапентин здається безпечним та ефективним при болю, пов’язаному з нервами. Як зазначає один експерт: «Оскільки весь біль зрештою передається нервами, популярність призначення ліків від нервового болю зростає». Обмежена доступність нових знеболювальних також сприяє цьому.
Габапентин відрізняється від опіоїдів тим, що не взаємодіє з опіоїдними рецепторами; натомість він уповільнює передачу нервових сигналів, впливаючи на кальцієві канали. На відміну від нестероїдних протизапальних засобів (таких як ібупрофен), які впливають на запалення, габапентин діє безпосередньо на самі нерви.
При Якому Болю Габапентін Дійсно Допомагає?
Хоча позареєстрове застосування широко поширене, ефективність габапентину варіюється.
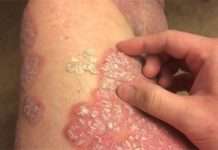
- Постгерпетична невралгія (ПГН): Це схвалене FDA застосування, що робить габапентин препаратом першого вибору при нервовому болю, пов’язаному з оперізуючим лишаєм.
- Синдром неспокійних ніг (СБН): Медичні рекомендації рекомендують габапентин як частину лікування СБН.
- Діабетична нейропатія: Хоча і не схвалений FDA для цієї мети, він часто рекомендується фахівцями з діабету як лікування першої лінії, хоча необхідні додаткові дослідження.
Однак докази ефективності габапентину при таких станах, як ішіас, мігрень та біль у попереку, слабші. Експерти застерігають від надмірної залежності від нього при цих проблемах через недостатні дані, що підтверджують. “Доказів, що підтверджують позареєстрове застосування габапентину при більшості клінічних станів… недостатньо”, – пояснює один дослідник.
Ризики, Побічні Ефекти та Кому Слід Уникати Його
Як і всі ліки, габапентин несе у собі ризики:
Загальні побічні ефекти: Сонливість, запаморочення, головний біль, розмитий зір, набір ваги.
* Серйозні ризики: Сплутаність свідомості, втрата пам’яті, утруднене дихання, синюшний відтінок шкіри (негайно зверніться за медичною допомогою).
* Потенціал зловживання: Поєднання габапентину з опіоїдами або седативними засобами збільшує ризик падінь та залежності, особливо у людей похилого віку.
Певні групи мають бути обережними:
- Старі люди: Підвищений ризик сонливості та падінь.
- Люди із захворюваннями легень або нирок: Можуть погіршити дихання або спричинити токсичність.
- ** Вагітні жінки: ** Обмежені дослідження вказують на потенційний ризик для плода.
Кому може принести користь Габапентін?
Габапентин може бути хорошим варіантом для людей із підтвердженими станами нервового болю. Однак обговоріть ризики та переваги зі своїм лікарем.
Замість того, щоб просто просити рецепт, поясніть, як біль впливає на ваше повсякденне життя. Також вивчіть інші варіанти: фізіотерапію, місцеві засоби, усвідомленість та зміни способу життя. Ліки можуть бути лише однією частиною головоломки.
«Іноді ліки допомагають пацієнтам навіть якщо вони призначені поза інструкцією, наприклад, габапентин. Важливо обговорити з лікарем співвідношення користі та ризику, щоб зрозуміти, чи підходить вам цей препарат».
Підсумок
Габапентин схвалений FDA для лікування судом, постгерпетичної невралгії та синдрому неспокійних ніг. Його позареєстрове застосування при інших больових станах поширене, але потребує ретельного розгляду. Якщо у вас нервовий біль, поговоріть зі своїм лікарем, щоб визначити, чи підходить вам габапентин.
Джерела: Див. оригінальну статтю для редакційних джерел.